Gut and the Brain Axis
In simple words, it’s a two way connection between the gut and the brain. This two way communication network includes the central nervous system (CNS), both brain and spinal cord, the autonomic nervous system (ANS), the enteric nervous system (ENS) and the hypothalamic pituitary adrenal (HPA) axis. What happens in our gut can directly influence our brain function and behavior.
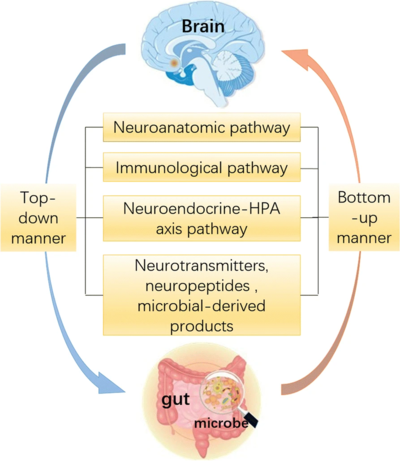
ANS is a component of the peripheral nervous system that regulates involuntary physiologic processes including heart rate, blood pressure, respiration, digestion and sexual arousal. It contains three anatomically distinct divisions: sympathetic, parasympathetic and enteric.
The enteric nervous system is composed of thousands of small ganglia that lie within the walls of the esophagus, stomach, small and large intestines, pancreas, gallbladder and biliary tree, the nerve fibres that connect these ganglia, and nerve fibres that supply the muscle of the gut wall, the mucosal epithelium, arterioles and other effector tissues.
What is microbiota?
It’s the symbiotic beneficial microorganisms present in our large intestine. A well-balanced beneficial interaction between the host and its microbiota is an essential requirement for intestinal health and the body as a whole. Under healthy conditions, the mucosal microbiota plays a vital role in food digestion, vitamin synthesis, angiogenesis, epithelial cell maturation, development, education of the host immune system and protection against pathogens.
What is the exact link between the brain and the gut?
● The gastrointestinal tract is connected to the brain through the vagus nerve. The vagus nerve links the heart, gastrointestinal tract and lungs to the brain (like a cable that connects all four). Sensory neurons carry feedback from the intestinal end to the brain stem which then engages the hypothalamus (which is a brain region that controls hunger and emotions) and limbic system (the emotional nervous system). Similarly, descending projections from the limbic system (activated via stress) influence autonomic activity of the gut.
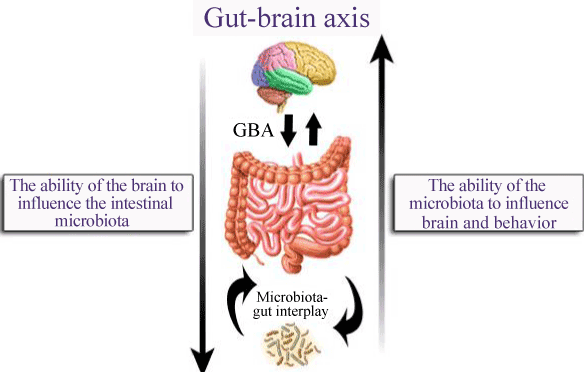
● Many species of Lactobacillus and Bifidobacterium produce gamma-aminobutyric acid (GABA), which is the main inhibitory neurotransmitter in the brain. Other bacteria have been shown to produce the neurotransmitters serotonin and dopamine. Bacteria also produce short-chain fatty acid that is able to stimulate the sympathetic nervous system, mucosal serotonin release and thus influence the memory and learning process in the brain.
● Gut microbial alteration, also known as dysbiosis, is a condition associated not only with gastrointestinal disorders but also with diseases affecting other distal organs. Recently it became evident that the intestinal bacteria can affect the central nervous system (CNS) physiology and inflammation. This dysbiosis, the two way connection between the brain and gut is dysregulated and associated with altered permeability of the blood-brain barrier (BBB) and hence neuroinflammation.
● The enteric nervous system (ENS), which is embedded in the lining of the gastrointestinal system, can operate independently of the brain and the spinal cord. The ENS is sometimes called the “second brain” because it contains such a diversity of neuron types, profusion of glial cells, and complex, integrated neural circuits. Its estimated 200–500 million neurons is roughly equal to the number in the spinal cord. The ENS functions to control bowel motility, secretion and blood flow to permit fluid and nutrient absorption and to support waste elimination.
● Accumulating evidence suggests that microbiota is involved in the physiology and pathology of cellular organisms and hence has implications in both health and disease. This distinct microbial flora, which is inherited maternally at birth, changes due to our dietary habits and environmental signals. The role of microbiota in various physiological activities, including in the immune system, has been well established. Several neurotransmitters and metabolites such as essential vitamins, secondary bile acids, amino acids and short-chain fatty acids (SCFAs), modulate many immune system pathways that in turn influence behavior, memory and learning, locomotion and neurodegenerative disorders. Among those pathways, researchers showed that the inflammation plays a role in depressive- and anxiety-like behaviors and locomotor activity.
As the details of gut-brain axis are still unclear however, it’s critical for future studies to clarify specific mechanisms by which gut microbes contribute to the progression or regression of certain pathological conditions which might further help in treating and diagnosing various disease conditions.
References:
https://www.sciencedirect.com/topics/neuroscience/enteric-nervous-system
https://www.physio-pedia.com/Gut_Brain_Axis_(GBA)
https://jneuroinflammation.biomedcentral.com/articles/10.1186/s12974-019-1434-3
Tags: Two way connection between gut and the brain, central nervous system (CNS), brain and spinal cord, autonomic nervous system (ANS), the enteric nervous system (ENS), the hypothalamic pituitary adrenal (HPA) axis, influence our brain function and behavior, peripheral nervous system, sympathetic, parasympathetic and enteric, microbiota, symbiotic beneficial microorganisms, the mucosal microbiota, vital role in food digestion, vitamin synthesis, angiogenesis, epithelial cell maturation, development, education of the host immune system, and protection against pathogens, link between brain and gut, Vagus nerve, hypothalamus, gamma-aminobutyric acid (GABA), inhibitory neurotransmitter in the brain, neurotransmitters serotonin and dopamine, dysbiosis, central nervous system (CNS) physiology and inflammation, neuroinflammation, second brain, short-chain fatty acids (SCFAs).